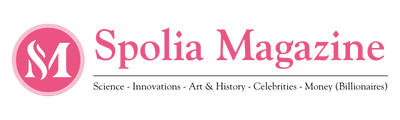Do you have stubborn acne that just refuses to go away? You’ve done everything you could think of but you still can’t get rid of it? Well, chances are you have fungal acne. No need to panic, it isn’t nearly as harmful as it sounds.
According to an estimation, about 10% of people worldwide suffer from acne at any given moment. It is the 8th most widespread disease in the world. Most commonly, it affects teens during puberty but it can occur at any stage in time if an individual doesn’t take care of their health, hygiene, and diet properly. Plus, there are different types of acne. Understand your condition better before treating it.
What is Fungal Acne? Is it different from Regular Acne?
Fungal acne is a skin condition caused by the overgrowth of yeast that is usually present in our hair follicles. We commonly call it Malassezia folliculitis or Pityrosporum folliculitis. Calling it acne is actually incorrect because, unlike acne, bacteria do not cause it. However, that does not mean it causes any less anxiety than regular acne does.
Since it’s different from the other forms of acne, it also has a distinctive treatment. Moreover, you cannot cure it with regular acne medications. Unfortunately, however, fungal acne often gets mistaken for acne vulgaris. So, we can never administer the appropriate treatment immediately. It isn’t really a surprise since the two are sometimes difficult to tell apart.
So, what does fungal acne look like? What are its symptoms and causes? How can you prevent it? This article answers all of your questions.
What Does Fungal Acne Look Like?

Fungal acne is very similar in appearance to regular acne which most people experience in their teens or early adulthood. While it is the same size and shape as acne vulgaris, some tell-tale signs can help you distinguish between the two.
First, the location of the fungal acne breakout is itchy while, with regular acne it is not. Secondly, this type of acne has uniform bumps that look like whiteheads. On the other hand, regular acne has bumps of varying size and appearance, occasionally occurring in clusters.
You are likely to find fungal acne on the back, chest, shoulders, and upper arm region. It also grows on oil-rich regions of your face such as the forehead, chin, and sides of your nose. Bacterial acne will grow on the face more often and is not as common in less-oily regions.
Lastly, while fungal acne does cause itchiness along with a burning sensation, it is not inflamed and will usually not have redness around it. Regular acne, however, has a lot of redness around the lesions.
While you should be able to identify the type of acne you have by understanding these differences, it is better to consult a dermatologist.
Diagnosing Fungal Acne:
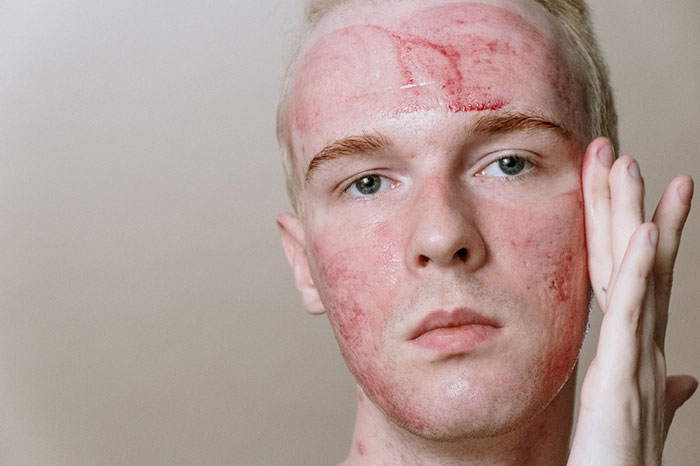
Getting a confirmed diagnosis of fungal acne is vital before you start taking medication. Medicines or antibiotics that you use for bacterial acne can worsen fungal acne and cause inflammation. Therefore, it is wise to go see a dermatologist for a diagnosis.
In most cases, the doctor will be able to determine the type of acne by knowing the answers to the following:
- How long do you have the lesions and breakouts?
- How has it responded to the treatments, you have tried?
- What symptoms are you experiencing with the condition?
In some cases, your dermatologist might also want to get a skin scraping to examine the sample and see if there is any yeast or fungi in it. They may also choose to do a simple biopsy to draw a more reliable conclusion.
What Causes Fungal Acne?

As mentioned earlier, fungal acne is a result of the excess growth of a fungal (or yeast) organism known as Pityrosporum. It is a part of our skin’s normal flora yet, this fungus exists in a proper balance with the bacteria of your microbiome (a community of micro-organisms living together).
Under certain circumstances, the skin loses this balance and it results in the eruption of fungal acne. There can be many reasons for this imbalance. We will discuss a few of these here:
1. Heat and Humidity:
Hotter climates are more likely to trigger and aggravate fungal acne. It is primarily because the yeast that causes this disease thrives in warm and moist environments.
2. Sweating:
Sweating exacerbates fungal acne since yeast grows better in moist places. All the following can cause fungal acne:
- Not showering after excessive sweat breakouts
- Not changing out the workout clothes after exercise
- Not washing sweaty clothes before reusing them
Moreover, wearing non-breathable fabrics that cling to your skin will also foster the perfect environment for yeast to grow on your skin.
3. Overuse Of Medication:
The bacteria on your skin keep the yeast population in check. When the population of bacteria gets disturbed, the yeast flourishes, thus leading to fungal acne. One cause of this is the prolonged use of topical or oral antibiotics.
4. Direct Contact:
It is possible to get fungal acne from someone who is already experiencing this condition since it is contagious.
5. Immunocompromisation:
With a weak immune system, you are more likely to suffer from fungal acne. This type of acne is common in people who recently have had surgeries, transplants, etc. These treatments could have weakened their immunity against fungal acne.
6. Irregular Diet Changes:
While no specific diet like keto or soup and salad diet could cause this condition, this disorder can aggravate by an excess of sugar or carbohydrates in your diet. Both of those substances are ideal food for fungi growth. According to a study, people who consume added sugars and cakes regularly showed a 20% to 30% greater risk of developing acne problems.
Similarly, fast food consumption is strongly linked with acne and obesity in the western world. Understandable, as fast food is rich in carbs, fats, and sugars.
7. Face Masks:
Face masks are a necessity nowadays due to the ongoing pandemic. Most of these masks are for single use only and are made of a material that traps heat and humidity under it. Therefore, they cultivate the ideal grounds for fungal acne to grow. In fact, skin disorders due to continued face mask use are so prevalent that there is even a name for this phenomenon – Maskne.
Read More: Easy Exercises to Tone up your Body Quickly
8. Steroid Induced Acne:
Steroids such as corticosteroids, steroid inhalation, topical steroid creams, and other bodybuilding drugs cause fungal acne. It is because when you take steroids, your body’s sebaceous glands release more oils, which the yeast feeds on.
Read More: Diamond Push-up
When Should You Visit A Doctor For Your Acne?
Acne is a common problem and nearly everyone experiences it once in his or her life. Consequently, you do not have to see a doctor about an issue so trivial. Nevertheless, if the breakout has not responded to your topical treatment in over 3 weeks, it is time to give your dermatologist a call.
Another reason for concern: the breakout subsides temporarily but returns to the same location shortly after. It might seem unnecessary at the time but a good antifungal treatment will not only cure the disorder but will also help prevent further breakouts.
Treating Fungal Acne:
Fungal acne is easy enough to treat. However, most people ignore the issue until it becomes serious. Fungal acne is very similar to regular acne and is often mistaken for it. So, most people often try to treat it like normal acne. Those treatments do not, however, work on fungal acne, and can end up making it worse.
The suitable way of dealing with fungal acne is by restoring balance to the skin’s flora. There are several ways to do this. While you could administer some of the treatments yourself, it is best to get a doctor’s opinion on other more serious ones
1. Anti Dandruff shampoos:
Anti-dandruff shampoos usually contain antifungal substances known as zinc pyrithione or selenium sulfide. A more potent antifungal chemical is ketoconazole. Shampoos and creams with this ingredient are only available as a prescription. Nevertheless, they are more effective than regular anti-dandruff shampoos. All in all, shampoos featuring such ingredients are great for combating fungal acne outbreaks. What you need to do is apply the shampoo to your skin and let it sit for a few minutes. Lather and rinse it off. You could make a habit of using it once a week as a preventive measure too.
2. Over-the-counter ointments:
Many OTC creams will specifically fight fungal growth. Products with ingredients such as ketoconazole, butenafine, or clotrimazole treat fungal diseases like athlete’s foot, jock’s itch, and others. You can use these to deal with fungal acne, as well. The skin on your face is more sensitive than that on the rest of your body. So, be a little more careful with what you use on your face.
3. Oral medication:
Drugs such as itraconazole or fluconazole target hair follicles and eliminate the infections in them. These are effective treatments but you might need a proper prescription for them.
4. Tea Tree Oil:
Tea tree oil is well-known for its antiseptic and antifungal properties. Hence, it is no surprise that it is a popular treatment option for fungal acne. To apply topically, you have to mix the tea tree oil with a carrier oil in a 1-2:12 proportion. The carrier oil can be any of your choosing such as olive oil, coconut oil, etc.
Since oils aren’t suitable for fungal acne, it is better to combine tea tree oil with salicylic acid. You can also combine it with benzoyl peroxide. It will increase the penetrative ability of the oil into the clogged pores. Tea tree oil can cause an allergic reaction in certain people, so make sure to perform a patch test before using it.
How Long Does Fungal Acne Last?
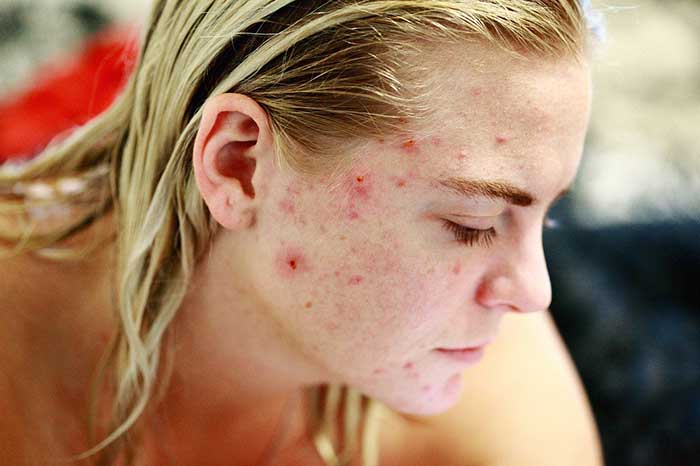
Left untreated, fungal acne can last weeks, months, and even years. With the right treatment, you will notice your skin healing within the first few days. Moderate occurrences of fungal acne will improve significantly in a matter of weeks but more severe cases can take longer.
How to Prevent Fungal Acne?
While there is no surefire technique to avoid fungal acne in its entirety, there are ways to lower the chances of getting it.Fungal acne is easy enough to treat
Avoid tight-fitting clothes:
Clothes that trap moisture and restrict airflow will lead to yeast growth on the skin. Wearing breathable fabric combats this and prevents excessive moisture accumulation. If avoiding tight clothing is not an option, you should make a habit of changing them immediately after use. Also, wipe off excessive sweat before changing into more comfortable clothes. Opt for loose clothing especially after workouts and during the acne treatment period to avoid aggravating it further.
Avoid Sugary Foods and Carbohydrates
Eating a well-balanced diet has numerous health benefits. Since excessive sugar leads to acne breakouts, it is imperative that you avoid it. Try low-fructose fruits instead for better nutrition as well as skin benefits.
Don’t Stress!
Usually, acne affects teens the most. However, adults are also susceptible to it too. There are numerous factors that lead to acne in adults. Some of them are menopause, smoking, genetics, diet as well as stress. Stress is particularly bad for acne. It might not directly cause it but hormone changes due to stress definitely intensify acne problems.
Take Showers Regularly
Hygiene is extremely important in preventing all kinds of acne. Make sure you shower regularly to get rid of excessive sweat as well as cleanse your face properly after wearing makeup all day. Makeup can also get stuck inside your pores and block them, leading to acne.
The Bottom Line
Fungal acne can be both painful and uncomfortable. It is easy to prevent it rather than treat it after it has gotten out of hand. Practicing good health and hygiene is the key to an acne-free body.